
AI-Powered Data Integration: Case Studies in Healthcare
Healthcare Technology
Updated Mar 28, 2026
Case studies showing how AI consolidates fragmented healthcare data to improve care, efficiency, and reduce costs.
Healthcare organizations struggle with fragmented patient data spread across multiple systems, leading to inefficiencies and compliance challenges. AI-powered integration is transforming this landscape by consolidating data into unified records, enabling better clinical decisions and operational improvements.
Key outcomes include:
Improved Patient Care: Predicting risks like sepsis and readmissions earlier.
Operational Efficiency: Cutting manual tasks by up to 90%.
Cost Savings: Annual savings ranging from $1.15M to $4.5M.
Case studies highlight successes such as Moorfields Eye Hospital achieving 94% diagnostic accuracy, University of Florida Health reducing clinician burnout, and Mayo Clinic cutting readmission rates by 25%. AI tools like NLP and machine learning streamline data handling, saving time and boosting accuracy. These technologies are reshaping healthcare by turning scattered data into actionable insights.
Role of Data and Interoperability in Effective AI in Healthcare
Case Studies: Healthcare Organizations Using AI for Data Integration
Here are a few examples that highlight how AI-driven solutions are addressing both clinical and operational challenges in healthcare.
Improving Diagnostic Accuracy with Retinal Imaging Data
Moorfields Eye Hospital in the UK teamed up with DeepMind Health in mid-2016 to tackle a pressing issue: the growing number of optical coherence tomography (OCT) scans far exceeded the capacity of human experts to interpret them. Each week, the hospital handles over 5,000 OCT scans, creating a significant bottleneck. As consultant ophthalmologist Dr. Pearse Keane explained, "Our eye scan volume outpaces human interpretation" [2].
To address this, Dr. Keane and Professor Sir Peng Tee Khaw led a project over five years, sharing one million de-identified eye scans to train a machine learning algorithm. The result? The AI system achieved an impressive 94% accuracy in identifying signs of more than 50 eye diseases and making referral recommendations [2][6]. This precision is critical, especially when considering that nearly 200 individuals in the UK are diagnosed daily with a blinding form of macular degeneration, while conditions like wet age-related macular degeneration and diabetic retinopathy affect over 625,000 people across the country [6]. To maintain patient trust, the project adhered to strict de-identification protocols, offered an opt-out option, and ensured data was destroyed securely using an 8-pass certified process.
This groundbreaking work has become a benchmark for AI applications in healthcare.
Clinical Decision Support at University of Florida Health
University of Florida Health has leveraged AI to integrate electronic health records with real-time clinical data, streamlining processes and improving accuracy. By employing natural language processing, the system automated time-consuming record-keeping tasks, a major source of clinician burnout. It also identified eligible patients for clinical trials, enhancing research capabilities [5].
What sets this system apart is its use of explainable AI, which provides transparency by showing the data behind its recommendations [6]. By automating routine documentation, clinicians could focus more on patient care and complex decision-making. The integration of real-time clinical records highlights AI's potential to deliver more comprehensive patient insights.
Operational Improvements at University of Rochester Medical Center
The University of Rochester Medical Center combined AI with ultrasound imaging and operational data to boost efficiency across its departments. The results were striking: manual effort dropped by 88%, decision-making sped up by 45%, case review completion rates jumped from 60% to 100%, and the time needed to search for scans shrank from 3–4 minutes to less than one minute [4][3].
These improvements not only saved time but also optimized resource use, showcasing how AI can drive measurable performance gains in healthcare settings.
Measurable Outcomes: Key Metrics Across Case Studies
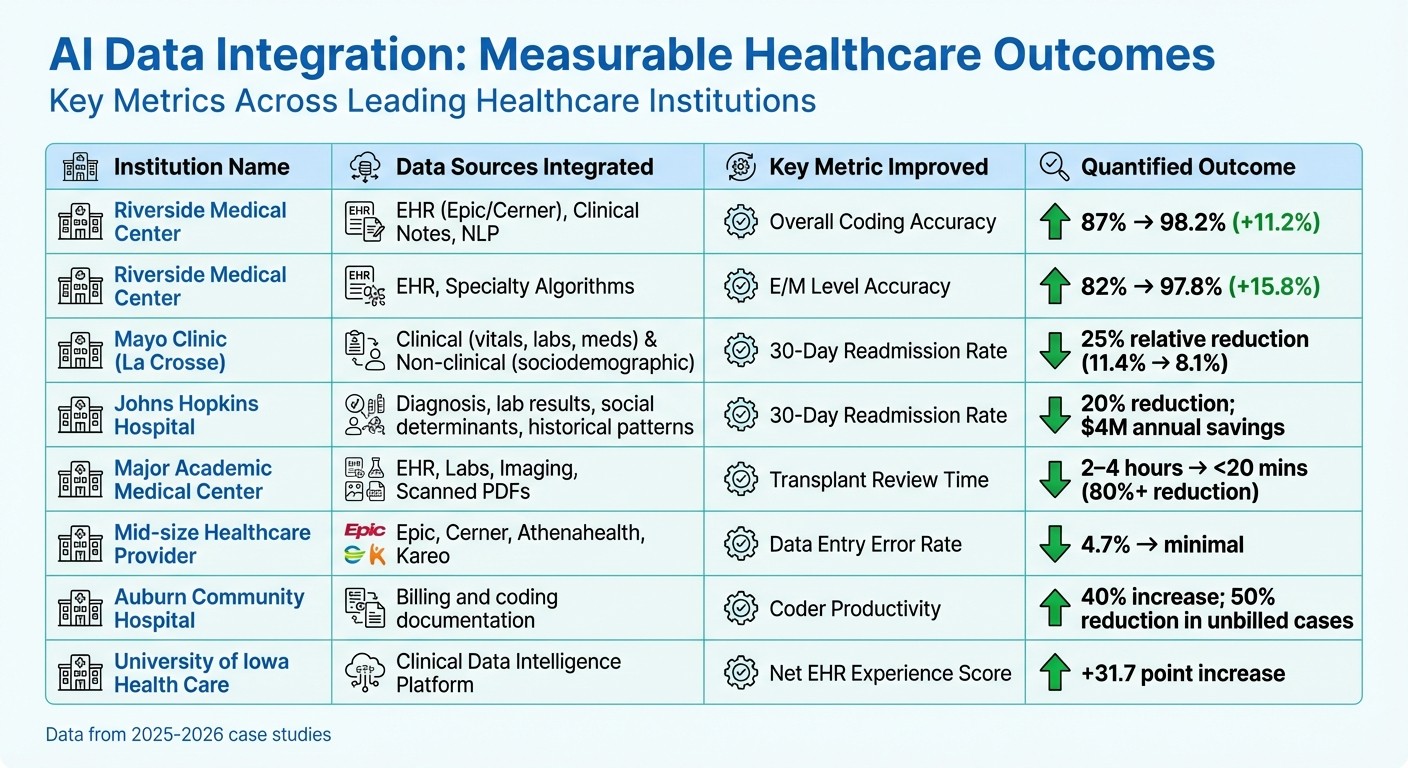
AI-Driven Healthcare Data Integration: Key Metrics and Outcomes Across Leading Institutions
Healthcare organizations that adopted AI-driven data integration systems have seen measurable gains in clinical precision, operational workflows, and financial results. Let’s dive into some specific examples that highlight these improvements.
Riverside Medical Center in California provides a compelling example. By introducing an AI platform in December 2025 that combined EHR data with natural language processing (NLP) for analyzing clinical notes, this 200-physician group achieved remarkable progress. Over a year, their overall coding accuracy jumped from 87% to 98.2%. Similarly, Evaluation and Management (E/M) level accuracy rose from 82% to 97.8%, a leap of 15.8 points. The platform also slashed coding time per encounter from 8 minutes to just 2.2 minutes, resulting in a 412% ROI and $1.7 million in annual savings [7].
At Mayo Clinic Health System's La Crosse Hospital, an AI system powered by XGBoost models analyzed data from 2,460 hospitalizations between 2025 and 2026. This initiative led to a 25% relative drop in 30-day readmission rates, reducing them from 11.4% to 8.1%. Researchers noted that patients assessed using AI were 47% less likely to be readmitted within 30 days compared to those receiving standard consultations. This reduction saved the hospital nearly $109,000 in care costs [10].
In another example, a major academic medical center optimized their transplant evaluation process by integrating AI to consolidate data from EHRs, lab results, and scanned PDFs. This reduced evaluation times from 2–4 hours to under 20 minutes - an efficiency improvement of over 80%. A surgical leader from the facility shared:
"Evaluating the referral records for a transplant candidate, which used to take hours, now takes less than twenty minutes, saving time, increasing productivity and throughput, and improving satisfaction" [8].
The table below outlines key metrics and results across these institutions:
Metrics Comparison Table
AI Integration Methods for Healthcare Businesses
Healthcare leaders are now tapping into advanced AI methods to streamline and expand data integration efforts, building on previous clinical and operational successes.
Using NLP and Machine Learning for Data Consolidation
Natural language processing (NLP) and machine learning are game-changers when it comes to organizing scattered healthcare data. These technologies take unstructured records and turn them into structured, actionable insights.
For instance, Capital District Physicians' Health Plan Inc. used Amazon Comprehend Medical and Textract to process over 7 million historical records. This effort led to a 60% efficiency improvement, cutting HEDIS reporting time from 4–5 days to twice daily. By standardizing data formats, the organization could analyze data from 3,000 electronic health records weekly using machine learning models [13].
Similarly, Atria Healthcare teamed up with GoML and applied Generative AI to patient data stored in Amazon S3. This approach improved risk prediction by 50%, reduced processing time by 45%, and increased diagnostic accuracy by 35% [12].
While consolidating data is a crucial first step, scaling these AI tools is just as important for gaining deeper insights.
Scaling AI Solutions for Complete Insights
To scale AI effectively, healthcare organizations need modular, serverless architectures that can handle growing data demands. The key is to start with high-impact use cases and integrate AI with existing systems rather than overhauling entire technology stacks.
Beacon Health System offers a great example. By implementing Xsolis' GenAI solution, they automated medical necessity reviews, slashing review times from 15 minutes to just 4.7 minutes - a 69% reduction. Payer approval wait times for three national payers dropped from 5 days to 2 days. Since 2019, this collaboration has saved Beacon over $95 million in operational costs [14]. The GenAI solution also brought consistency to nursing teams, ensuring all reviews were backed by comprehensive information.
For organizations looking to scale AI, making data accessible to frontline staff is essential. Quality filters with accuracy scores ensure only reliable data enters clinical workflows. Feedback loops, such as asking clinicians whether AI insights met their needs, help fine-tune the models over time. Additionally, for managing both clinical data and patient communication, tools like Lead Receipt's AI-powered receptionist can handle routine tasks like scheduling and intake, freeing staff to focus on more complex care.
These AI integration strategies allow healthcare organizations to turn fragmented data into meaningful insights, improving patient care and operational performance.
Conclusion
The case studies highlight how AI-driven data integration is reshaping both clinical and operational aspects of healthcare. For instance, Beacon Health System managed to cut review times by an impressive 69% [14], while Regional Medical Center improved cash flow by $10.7 million [1]. These achievements reflect advancements in both clinical quality and revenue cycle performance.
Organizations adopting AI solutions have also seen a dramatic drop in administrative workloads. For example, one healthcare provider reduced its work order backlog from 850 to 220 orders within just 90 days, and clean claims rates jumped from 82% to 91% [1]. Cone Health achieved a 0.93 mortality observed-to-expected ratio, placing it among the top 10% for mortality outcomes [15]. These results demonstrate how AI integration can enhance both financial operations and patient care quality.
Starting small can be a smart strategy for organizations new to AI. A focused pilot program allows healthcare providers to validate results using real baseline data. Leveraging pre-built integrations with platforms like Epic or Cerner can further streamline the process, cutting implementation time to as little as two hours [9] without requiring a complete technology overhaul.
AI's potential goes beyond clinical data. Tools like Lead Receipt's AI-powered receptionist handle routine tasks around the clock, enabling clinical staff to focus on more complex care. This dual benefit - automating data management while enhancing patient engagement - makes AI an essential tool for modern healthcare operations.
The results speak for themselves: tailored AI solutions not only elevate patient care but also deliver measurable operational savings. As the CFO of Regional Medical Center shared after achieving a 56X ROI in just 90 days:
"This is the first time in my 15 years as CFO that a vendor showed me ROI with OUR actual data, not industry benchmarks. The transparency of the dashboards and the rigorous measurement methodology gave me confidence." [1]
At this point, the question isn’t whether to implement AI, but how quickly healthcare organizations can take advantage of these transformative improvements.
FAQs
What data sources should we integrate first for the fastest impact?
To make a quick impact, focus on integrating AI-driven patient communication and scheduling tools with existing EHR systems such as Epic, Cerner, or Athenahealth. Pairing these systems with scheduling platforms helps streamline workflows, cut down on manual tasks, and boost overall efficiency, all while enhancing the patient experience.
How do healthcare teams keep patient data private when using AI?
Healthcare teams safeguard patient data by adopting on-premises AI solutions that align with regulations like HIPAA. They take critical steps such as maintaining detailed audit trails, ensuring data sovereignty, and adding custom security layers to block breaches and unauthorized access. These measures allow sensitive information to stay secure while benefiting from AI advancements.
How do we validate AI results before putting them into clinical workflows?
Healthcare organizations ensure the reliability of AI results in clinical workflows by leveraging clinical decision support systems, analyzing peer-reviewed case studies, and adhering to regulatory standards. These measures are crucial for verifying the accuracy, security, and interoperability of AI-generated outputs prior to their implementation.