
AI Agent Workflows: Case Studies in Healthcare
Healthcare Technology
Updated Mar 14, 2026
AI agents are transforming healthcare operations by automating scheduling, documentation, and intake—cutting costs, reducing burnout, and improving patient satisfaction.
AI agents are reshaping healthcare by automating time-consuming tasks, reducing costs, and improving patient experiences. From appointment scheduling to documentation and lead management, these tools are tackling inefficiencies and staff burnout. Here's what the article covers:
Case Study 1: A regional health center reduced its no-show rate by 78% and cut administrative costs by 89% using AI for 24/7 scheduling and reminders. Patient satisfaction jumped from 72% to 95%.
Case Study 2: A multispecialty hospital cut documentation time by 37.59%, enabling physicians to treat 18.36% more patients with real-time AI-powered clinical notes.
Case Study 3: Home care agencies saved $800,000 annually and reduced scheduling delays from three days to 28 minutes with AI receptionists.
Key takeaways:
AI integration with EHR systems boosts efficiency and reduces staff workload.
Phased rollouts and staff collaboration are critical for smooth adoption.
Security and compliance, like HIPAA standards, are essential for patient trust.
AI's role in healthcare is expanding, with future advancements focusing on real-time patient monitoring and multi-agent ecosystems for complex workflows.
Case Study 1: AI Scheduling Automation at a Regional Health Center
Problems Before AI Implementation
The Regional Medical Center, a 500-bed facility catering to 200,000 patients annually, struggled with an overwhelming administrative workload. Handling over 2,000 calls daily for appointments and inquiries, the front desk staff faced constant pressure, resulting in long wait times for patients. Operating hours were limited to the standard 9–5 window, leaving many patients unable to schedule appointments after work hours. Administrative employees spent a staggering 70% of their time on repetitive tasks like manual scheduling and addressing routine questions. This not only led to burnout and high turnover among staff but also contributed to operational inefficiencies. The center experienced a 25% no-show rate and a patient satisfaction score that hovered at a concerning 72% [8].
To tackle these challenges, the center turned to an AI-driven scheduling solution.
AI Agent Implementation and Results
In late 2025, the center began a 10-week phased rollout of Lead Receipt's AI automation platform, seamlessly integrating it with their Electronic Health Records (EHR) system. The AI system took over routine inquiries and automated appointment scheduling, providing patients with 24/7 access to booking services. This shift brought significant improvements across the board.
Within just six months, the no-show rate plummeted from 25% to 5.5% - a dramatic 78% decrease - thanks to automated reminders sent via SMS, email, and voice calls. The AI agent now handles 85% of routine inquiries, allowing administrative staff to focus on more complex and high-priority patient needs. These changes not only improved internal operations but also had a noticeable impact on patient experience. Patient satisfaction soared from 72% to 95%. On top of that, the center saw an 89% reduction in administrative costs and a remarkable 300% boost in patient leads [8].
Jennifer Walsh, Patient Services Manager, shared her thoughts: "The appointment scheduling has become so much smoother. Patients love being able to book appointments at any time, and the automatic reminders have virtually eliminated our no-show problem."
Case Study 2: Reducing Documentation Work with AI at a Multispecialty Hospital
Addressing Documentation Overload
Billings Clinic – Logan Health, a network of 25 hospitals serving 1,200 physicians across 80 specialties in Montana and Wyoming, faced a serious challenge: overwhelming documentation demands were straining their staff and impacting patient care. Physicians were bogged down with manual note-taking during patient visits, all while managing constant interruptions from calls and emails. This workload often forced clinicians to skip breaks and work late into the evening just to keep up [9].
Each patient consultation required an additional 10–15 minutes for documentation [10]. Nurses spent nearly 40% of their workweek - around 16 hours - on paperwork, taking time away from direct patient care [12]. On top of this, manual record routing delayed access to critical patient information by 8–12 hours, hindering team coordination [12]. After clinic hours, providers often spent over an hour completing routine charting tasks [11].
"Such administrative work left the group's physicians feeling fatigued and dissatisfied", the hospital reported [9].
To tackle these challenges, the clinic turned to an AI-driven solution.
How AI Agents Improved Efficiency
Between February 2024 and April 2025, Billings Clinic implemented the Oracle Health Clinical AI Agent across its physician network, transforming how documentation was handled. This advanced AI system used natural language processing to capture patient-physician conversations in real-time. It could distinguish between medical history and current symptoms, organizing the information into structured clinical notes. These notes were then seamlessly integrated into the Oracle Health Foundation EHR system [9].
The impact was substantial. The clinic reduced average documentation time by 37.59% and cut time spent in the EHR per patient by 16.69%. Physicians who relied on the AI agent for at least 75% of their notes saw an 18.36% increase in the number of patients they could treat [9]. These gains eased the interruptions and after-hours workload that had previously drained staff. Dr. Randy Thompson, Chief Health Analytics Officer, shared the reasoning behind their choice:
"We chose Oracle Health Clinical AI Agent because it demonstrated it could actually reduce the burden of documentation" [9].
With the AI system in place, providers could complete their notes almost instantly - often finishing before their next patient arrived. The technology removed the documentation roadblock that had previously distracted providers, enabling them to focus fully on their patients rather than on screens and keyboards. As seen in other examples throughout this article, the integration of AI not only streamlined operations but also elevated the quality of patient care.
Case Study 3: AI Receptionists for Lead Management in Home Care Agencies
Lead Management Problems
Home care agencies often struggle with managing high call volumes, leading to missed opportunities and inefficiencies. For instance, one major home health provider dealt with 21,000 calls every month, yet about 50% of calls transferred to local branches ended up in voicemail[14]. Adding to the challenge, manual pre-admission and intake processes could take as long as 20 minutes per patient, creating delays and limiting the ability to track follow-ups effectively[13][14]. Christopher Williams, President of Elite Web Professionals, summed up the impact of these issues:
"The AI Voice Receptionist has been a game changer. It gave us visibility into missed calls we never knew about - now we know who's calling, what they need, and we can follow up."[15]
To tackle these problems, many agencies turned to AI-powered receptionist systems.
Benefits of AI-Powered Receptionists
Lead Receipt's AI receptionist system was introduced to address these operational hurdles. This 24/7 platform ensures callers are attended to without delays or hold times[14]. Beyond answering calls, the AI handles several administrative tasks, such as collecting demographic information, verifying insurance, and scheduling appointments - all without requiring human input.
The impact was striking. One prominent home health provider saved over $800,000 annually by reducing the need for full-time staff to manage incoming calls[14]. The AI system resolved 27% of calls within 15 minutes, completely eliminating patient hold times. Agencies using AI for intake and surveys reported yearly savings ranging from $200,000 to $300,000[14][13].
Scheduling became significantly faster too - tasks that used to take three days were now completed in just 28 minutes. The system seamlessly integrated with platforms like Salesforce, syncing data in real time and avoiding duplicate entries. Even 27% of after-hours inquiries were captured by the AI, ensuring no potential lead slipped through the cracks[15]. Overall, agencies saw up to a 40% reduction in operational costs while boosting lead conversion rates.
Part 4: Real-World AI in Healthcare – Global Case Studies | Dr. Bharani Kumar Dupuru | ACCC’25 Day 2
Measured Results from the Case Studies
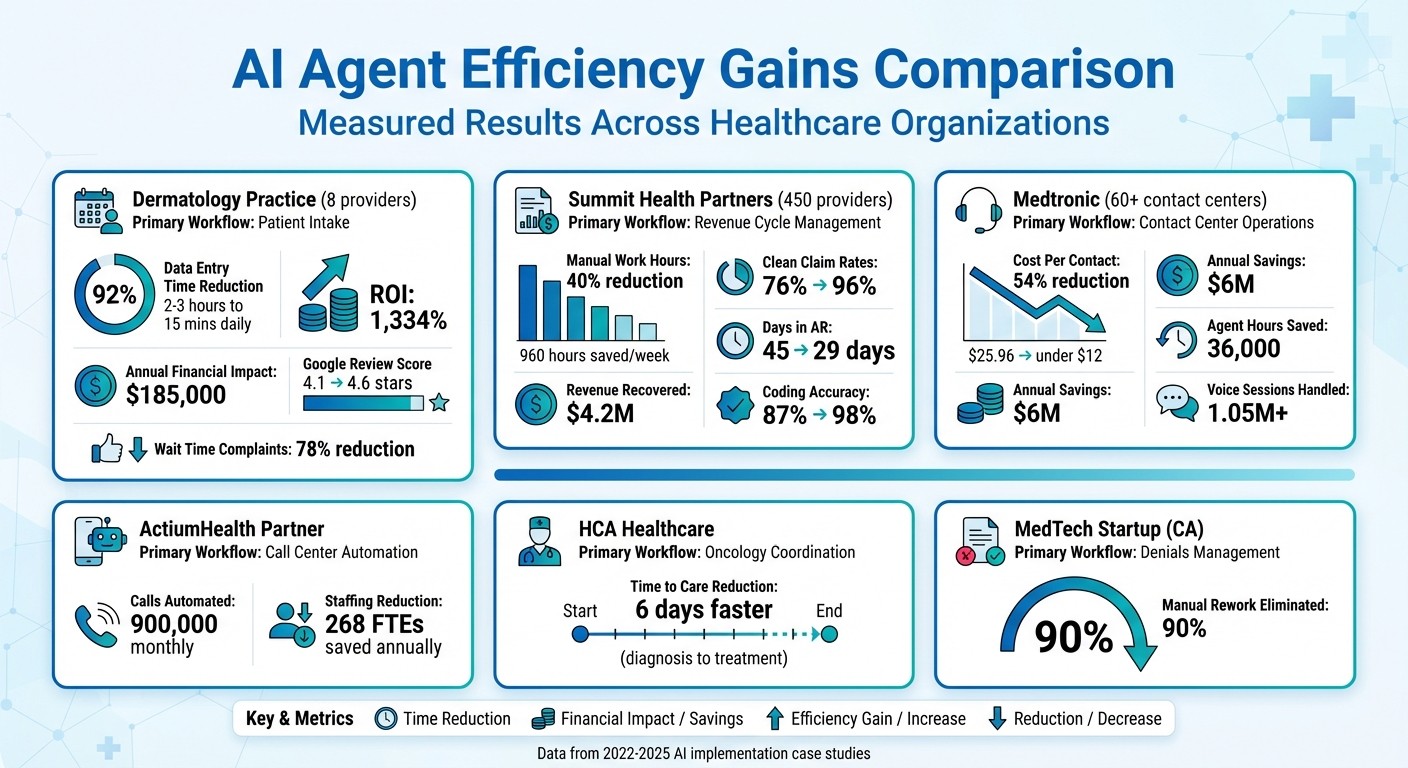
AI Healthcare Implementation Results: Efficiency Gains Across 6 Organizations
AI agents have delivered impressive improvements in operations, boosting both financial outcomes and patient satisfaction. The following examples highlight these advancements across various healthcare organizations.
A multi-location dermatology practice with eight providers managed to cut data entry time by an astounding 92%, reducing the process from 2–3 hours daily to just 15 minutes. With an initial investment of $12,900 in the first year, this efficiency generated an annual financial impact of $185,000 - a massive 1,334% return on investment. Additionally, their Google review score climbed from 4.1 to 4.6 stars, while complaints about wait times dropped by 78% [16].
At Summit Health Partners, a multispecialty group with 450 providers, AI agents helped recover $4.2 million in revenue. Clean claim rates rose from 76% to 96%, days in accounts receivable dropped from 45 to 29, coding accuracy improved from 87% to 98%, and registration errors decreased by 67% [2].
Between 2022 and 2023, Medtronic implemented AI agents in over 60 contact centers, handling more than 1.05 million voice sessions. This deployment saved the company $6 million and 36,000 agent hours, cutting the cost per contact from $25.96 to under $12 - a 54% reduction [18].
ActiumHealth Partner automated 900,000 calls monthly, saving the equivalent of 268 full-time positions each year [17].
Efficiency Gains Comparison
The table below provides a snapshot of key efficiency improvements across different organizations:
These examples highlight how AI-driven workflows can streamline operations, reduce costs, and improve patient care across various healthcare settings.
Implementation Guidance for Healthcare Businesses
Scalability and Integration Approaches
Rolling out AI in healthcare demands a phased, structured approach. Generally, organizations go through three main stages: Audit, Pilot, and Governance. During the Audit phase, teams identify workflows with the highest impact and estimate potential ROI - this takes about two weeks. The Pilot phase focuses on connecting two or three systems and automating one key workflow, delivering results within 4–6 weeks. Finally, the Governance phase ensures ongoing leadership involvement and scales the roadmap for broader implementation [1].
For AI to scale effectively, it must integrate seamlessly with existing systems. This often requires custom connectors for major EHR platforms like Epic, Cerner, Athenahealth, and Kareo to enable real-time data exchange. For example, in March 2025, a mid-sized U.S. hospital network collaborated with an automation provider to deploy three AI agents - AuthBot, Max, and ChartGenei - using custom connectors for Epic and Cerner. Within just eight weeks, these systems achieved HIPAA certification, reduced nurse burnout from 62% to 37%, and boosted staff retention from 68% to 89% [1].
Security is non-negotiable. AI systems must comply with HIPAA standards, using features like PHI tokenization and 256-bit AES encryption. Jennifer Davis, Cofounder and Co-CEO of Davis Osteopathic Center, highlighted the importance of this:
"The knowledge that Providertech employs HIPAA-compliant 256-bit AES encryption gives us great assurance that our communications with patients are fully secure in an age of constant digital threats" [19].
Another crucial element is establishing clear AI-to-human handoff protocols to maintain safety and trust. Staff should clearly understand when tasks need to escalate from an AI agent to a human team member. To streamline this, some organizations implement an orchestration layer - a centralized system that coordinates multiple AI agents across departments - making it easier to scale operations [1].
While integration is vital, success also hinges on managing change and ensuring staff buy-in.
Managing Change and Staff Adoption
Even with seamless integration, aligning staff and workflows is essential to sustain AI-driven improvements. The key to success? Involving frontline staff from the start. For instance, in March 2025, an automation provider conducted 23 co-design interviews with nurses and clinicians before launching their AI system. This collaborative process ensured the technology addressed actual pain points rather than creating new challenges [1].
Position AI agents as tools that assist staff, not replace them. At Davis Osteopathic Center in Indiana, the conversational AI agent "Grace" handles 77.4% of routine inquiries, allowing staff to focus on more complex patient care. This setup led to a 75% reduction in time spent manually confirming appointments [19].
Providing hands-on support during transitions is equally important. Jenny Smith, Senior Director of Digital Health at Franciscan Missionaries of Our Lady Health System, reported that such support reduced after-hours documentation by 65%. Additionally, 100% of surveyed clinicians noted improvements in their work-life balance [20].
To ease staff resistance, start with high-burnout areas. Tackling bottlenecks like prior authorizations, documentation, and call routing can quickly demonstrate the value of AI. For example, Summit Health Partners implemented a 16-week phased rollout, emphasizing change management and teamwork. This approach reduced manual work hours by 40% and lowered annual staff turnover from 65% to 32% [2].
For organizations lacking full-time automation leadership, fractional executives can be a cost-effective alternative. Notably, 73% of private equity-backed companies now use fractional leadership to guide their AI strategies without committing to a permanent hire [6].
Conclusion: What's Next for AI Agent Workflows in Healthcare
Main Lessons from the Case Studies
The case studies highlight three key factors that drive success when implementing AI in healthcare.
First, deep system integration is critical. Organizations that connected AI agents to their EHR systems saw major benefits, such as improved revenue recovery thanks to smoother data flow.
Second, phased rollouts work better than jumping straight into large-scale deployments. Starting with simpler, high-volume tasks - like appointment scheduling or eligibility checks - helps organizations build confidence and fine-tune workflows before tackling more complex clinical processes.
Finally, 24/7 availability fills an important gap. A large share of patient inquiries happens outside regular business hours. For example, at an Academic Medical Center in February 2026, AI-driven outbound calls brought in $39M in yearly revenue by scheduling over 49,000 additional appointments during off-hours [3][19][22].
These lessons lay the groundwork for healthcare organizations to embrace even more advanced AI capabilities.
Future Directions
The next wave of AI in healthcare is shifting from improving processes to actively enhancing patient care. AI agents are now monitoring medical devices and reaching out to patients when issues arise. For instance, Medtronic’s pilot program, "Virtual Earl", contacts patients based on device alerts, already saving $6M annually [5].
Agentic AI is leading the charge into the future. These sophisticated systems don’t just follow predefined scripts - they evaluate complex situations, coordinate between departments, and solve problems independently. Some organizations are even creating multi-agent ecosystems, where specialized AI handles tasks like eligibility checks, coding, and appeals, all managed through a central coordination system [21][2].
For healthcare providers ready to explore AI automation, solutions like Lead Receipt (https://leadreceipt.com) offer 24/7 AI receptionists and workflow tools that integrate seamlessly with CRMs and scheduling platforms. These tools make it easier than ever to adopt AI and streamline operations.
FAQs
What healthcare workflows should we automate first with AI agents?
Start with automating high-volume, repetitive tasks such as patient intake, appointment scheduling, and managing calls. For instance, AI-powered tools can help cut down patient wait times, reduce errors, and ease the workload on front desk staff. By automating processes like sending appointment reminders or conducting initial symptom checks, healthcare providers can boost efficiency and enhance the patient experience. These foundational steps can set the stage for integrating AI into more complex healthcare operations.
How do AI agents integrate with our EHR without breaking workflows?
AI agents connect with Electronic Health Records (EHR) through secure, context-aware systems that provide real-time access to data without interrupting daily operations. By leveraging robust APIs and reliable data exchange protocols, these agents ensure data remains consistent and accurate. This enables automation of tasks such as scheduling, documentation, and insurance verification. The result? Clinicians experience less manual workload, workflows become more efficient, and healthcare delivery stays smooth and uninterrupted.
How can AI agents stay HIPAA-compliant and protect PHI?
To keep Protected Health Information (PHI) secure and meet HIPAA requirements, healthcare organizations should focus on encryption, access control, and monitoring. Encrypting data both at rest and in transit with strong methods like AES 256-bit is a must. Adding role-based access control (RBAC) ensures that only authorized individuals can access specific data, while multi-factor authentication (MFA) strengthens login security.
Detailed audit trails help track who accessed what and when, which is crucial for accountability. Real-time monitoring of systems can detect potential breaches early, and establishing Business Associate Agreements (BAAs) with vendors ensures they also follow strict security protocols. For organizations looking to retain full control over sensitive data, on-premises AI solutions can be an effective option.